World Kidney Day was observed a few days ago. Due to the sharp rise of kidney diseases especially Chronic Kidney Disease (CKD) projected to be the 5th leading cause of death by 2040, compounded by the lack of knowledge at all levels, the International Society of Nephrology (ISN) this year declared that bridging the knowledge gap to better kidney care was the best way to help patients and improve their life’s quality.
To find out more about CKD, how it is caused, and how it can be prevented in high risk groups, the Sunday Observer spoke to Consultant Nephrologist, Sri Jayewardenepura General Hospital, Colombo, Dr Chinthana Galahitiyawa, to answer these questions uppermost in the minds of all those at risk of developing CKD, from his hands- on- expertise and knowledge gleaned over the years.
Excerpts
 Q. Although this year’s theme for World Kidney Day is “Kidney Health for all,” the focus is on Chronic Kidney Disease ( CKD) .Why? What is its significance to kidney patients worldwide and Lankans in particular?
Q. Although this year’s theme for World Kidney Day is “Kidney Health for all,” the focus is on Chronic Kidney Disease ( CKD) .Why? What is its significance to kidney patients worldwide and Lankans in particular?
A: Chronic kidney disease (CKD) was selected this year as our focus because it is becoming increasingly common, reaching pandemic levels. Worldwide, 10 percent of the adult population have it and is projected to be the 5th leading cause of death by year 2040. Hence,” Bridging the knowledge gap to better kidney care” was considered as the way forward by the International Society of Nephrology (ISN) for the year 2022. In the case of our own country, Sri Lanka’s disease burden is worse compared to some other countries compounded by a serious knowledge gap among the healthcare workers, general population and policy makers which makes our focus on bridging the knowledge gap all the more relevant.
Q. Although many people are familiar with the term chronic kidney disease they still don’t understand what exactly it means. So, briefly tell us where the kidneys are located and what their functions are in ensuring our health.
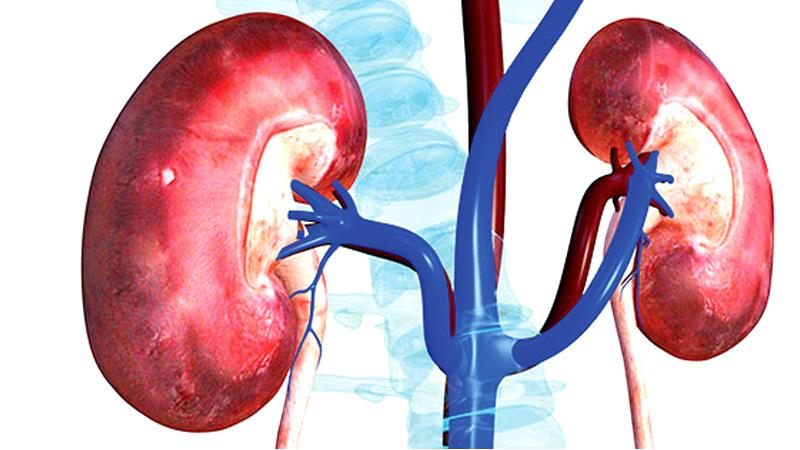
A: Kidneys are inside of the body at the loin region, more towards the back wall. Kidneys are responsible for clearing up of the blood from toxic metabolic waste products and maintaining water, electrolytes and acid-base balances. Kidneys produce a hormone called “Erythropoietin” which stimulates the bone marrow to produce red blood cells and contribute to producing vitamin D in the body. Gradual and irreversible loss of kidney functions over a period of time is called chronic kidney disease (CKD).
Q. How is CKD connected to creatinine and e-GFR?
A: Creatinine is a metabolic waste product principally cleared by the kidney and it is quantified by a biochemical test on a blood sample. When the kidney functions are gradually deteriorating in CKD, serum creatinine level gradually rises. Kidney function is measured and its progression is monitored by serial serum creatinine levels. e-GFR is the mathematical estimation of kidney function based on the serum creatinine level. When kidneys fail, serum creatinine will rise and the e-GFR will fall. Hence, e-GFR is inversely proportional to creatinine level.
Q. I understand there are two main kidney diseases. Is this correct?
A: The main types of kidney diseases are AKI (Acute Kidney Injury) and CKD. AKI is fast deterioration of kidneys within days with the potential to recover completely upon right treatment. The best example is dehydration resulting in AKI which is reversed with prompt hydration. CKD on the other hand is a slower process with gradual loss of kidney function over months to years. CKD is not reversible and can be slowed down or controlled if detected early.
Q. What are the most common causes for chronic kidney disease in Sri Lanka? Pre-existing Non Communicable diseases like diabetes etc?
A: Diabetes mellitus is the worldwide leading cause. High blood pressure, kidney infections, blockages, glomerular diseases, toxic drugs and chemicals and hereditary kidney diseases are among the other causes. CKD found in north central province has no definite cause found up to date.
Q. Other risk factors that lead to this disease?
A: As I said diabetes is the leading cause - specially uncontrolled sugar levels. Others include , uncontrolled high blood pressure, over consumption of painkillers, kidney stones and prostate enlargement, family history of CKD, obesity, smoking, presence of other chronic illnesses such as arthritis and residing in endemic areas of CKD are risk factors for CKD.
Q. Does genetics play a contributory factor? Can one inherit CDK?
A: Yes, certain CKDs are inherited. Example- polycystic kidney disease. Some people are also genetically at higher risk to develop kidney stones. Similarly, we observe certain families with diabetes showing fast deterioration of CKD reaching the end stage.
Q. Can you have a kidney disease without knowing it? If so, are there early signs to look out for?
A: As CKD slowly progresses, one’s body gets sufficient time to adjust for the biochemical changes. Therefore, most of the CKD patients are asymptomatic up until they reach the end stage. There are NO early signs for CKD. It needs screening of all high-risk categories on a regular basis. We recommend annual screening with a serum creatinine level and a urine full report.
Q. How does kidney disease affect the body?
 A: As kidney failure progresses, the internal environment gets unfavourable for the other cells and organs to function. Gradually the whole system becomes weak-specially organs such as heart and liver get affected. Ultimately, brain functions are affected and the patient develops confusion and fits. This can be fatal without prompt treatment.
A: As kidney failure progresses, the internal environment gets unfavourable for the other cells and organs to function. Gradually the whole system becomes weak-specially organs such as heart and liver get affected. Ultimately, brain functions are affected and the patient develops confusion and fits. This can be fatal without prompt treatment.
Q. Can CKD be cured?
A: CKD has No cure. It can only be controlled and slow the progression. Therefore, detection at an early stage is extremely important.
Q. Can drinking a lot of water help ?
A: Adequate water intake is important to maintain kidney health. We recommend drinking 2.5 litres for males and 2 liters for females. But, if you are working in a hot environment with much water being evaporated with sweat, you need more water to compensate.
Q. How is kidney disease diagnosed?
A: Basic kidney tests include serum creatinine level and urine full report. Other supportive tests include blood urea, serum electrolytes and ultrasound scan of kidneys. Early kidney damage in diabetics can be detected by urine micro-albumin level.
Q. Treatment wise – how is a kidney patient treated ? Walk us through the different stages of the procedure involved.
A: After initial confirming the diagnosis and staging, we need to look for the complications that have already happened. Most important aspect here is the education of the patient and the role of the caregivers as controlling the cause of the CKD is a priority. The patient is offered advice regarding his/her optimal diet, lifestyle and the water intake. Medical management and follow-up are planned according to the stage of the CKD. CKD-4 patients are counselled regarding the renal replacement therapy and prepared for it. CKD-5 patents also need close monitoring for initiation of dialysis or kidney transplantation.
Q. When does a patient need haemodyalisis ?
A: When the complications of advanced CKD cannot be controlled with medicines the patient needs dialysis. Example- uncontrolled high potassium levels, severe swelling of the body not responding to drugs.
Q. As we all know, preventing kidney disease is much less expensive and easier than treating it. So how do you prevent kidney disease in the first place?
A: This can be done by bridging the knowledge gap on CKD through community-based health education programs. The leading causes of CKD should be discussed widely through the media. Screening facilities should be made available easily.
Preventative strategies such as tight blood sugar control, optimal blood pressure control, healthy lifestyles are important. Hence promotional programs and regular periodic health education which are already in place should be made stronger and put into practise throughout the country.
Diagnosed patients should be treated at special community-based clinics at earlier stages and the advanced cases should be referred to specialised kidney units.
At the community level low CKD awareness, limited health literacy, limited availability of CKD information and lack of readiness to learn have been recognised as main obstacles. So we need to improve knowledge on CKD among the general population, health care workers and policy makers.
Healthcare workers need more focused education of CKD and its preventative measures. Public health policy makers should pay more attention to CKD as it is as much important as cardiovascular disease, cancer, diabetes and chronic respiratory diseases.
Q. Have you a word of advice to kidney patients and also those who are borderline cases?
A: Be informed about your kidney health. If you are a high-risk person for developing CKD, it is mandatory to screen annually. The high-risk categories for CKD include all diabetics, hypertensives, patients with kidney stones, patients with blood relations having CKD, living in CKDu endemic areas, obese, smokers, having any kind of chronic illnesses and all above 50 years of age.
If you are diagnosed to have any weakness of your kidneys, seek medical attention without neglecting them. All borderline cases should be followed up closely at medical clinics and if they show deterioration needs to attend specialised kidney care clinics.
Q. Anything else you wish to add?
A: Patients who reach advanced CKD stages need preparation for renal replacement therapy and when the right time comes they need to start dialysis and kidney transplant without undue delays. That said, at this point, I would also like to emphasise that Sri Lanka now has a well-established mainly public sector driven dialysis program delivered in more than 50 centers across the country. We have a very successful kidney transplant program with results parallel to developed countries. All anti rejection medicines are given free of charge for kidney transplanted patients. Further, as a solution to organ shortage for transplantation, a deceased organ donor program is established and carried out successfully.
Q. For more information on this subject is there a contact number?
A: You can get more information on kidney disease, organ donation and transplantation from the following links. www.odtf.lk, www.facebook.com/OrganDonorDaySL, www.facebook.com/odtf.lk/
